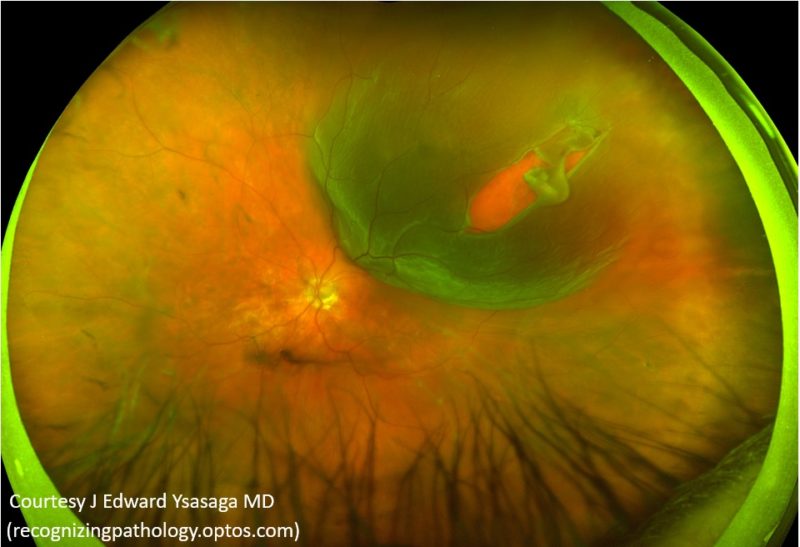 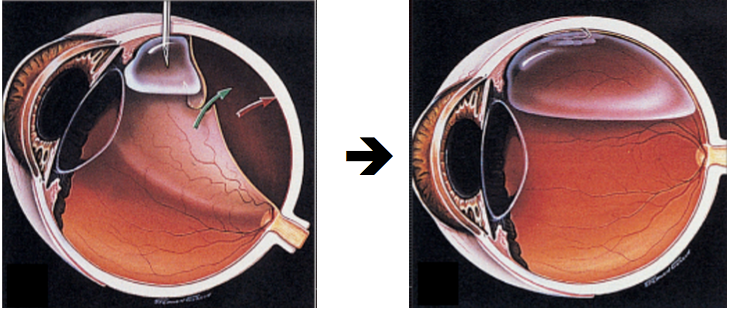
Furthermore, Wenkel and Naumann 13 reported the retrolaminar changes in the optic nerve after SO instillation with secondary angle-closure glaucoma. 2c).Īlazemi and colleagues 12 disclosed the direct migration of liquid SO from the breast to the mediastinum. SCI (Oculus) showed heterogeneous, highly reflective, tiny scattered areas in the upper half of the intrastromal space in OD ( Fig. On slit-lamp examination, haze on the upper half of the corneal stroma and intrastromal tiny, bright, and emulsified SO particles were noted. Intraocular pressure was 8 mmHg, vision remained hand movement. Six months later, mild corneal haziness developed. Slit-lamp examination findings on the first postoperative day and month were normal. Repeat vitrectomy, SO extraction, preretinal membrane peeling, internal drainage of subretinal fluid, endophotocoagulation, and intravitreal gas (C3F8) tamponade were performed. Five months later, retinal redetachment developed in the eye. At that time, the cornea was not injured and the retina was attached. 7 The SO bubble was removed spontaneously with this corridor.Ī 34-year-old man underwent 23-gauge vitrectomy, intraocular foreign body removal, and 1000-centistoke SO tamponade combined with phacoemulsification on his right eye due to scleral penetrating injury with a piece of metal wire. Additionally, air was then injected with a 30-gauge cannula between the deep stroma and Descemet membrane to separate those layers, as described previously. Intravitreal SO was removed via pars plana sclerotomies. SCI (Oculus) revealed a sharply demarcated, wide, hyporeflective area between the corneal stroma and Descemet membrane in the right eye ( Fig. The diameter of the bubble was about 6 mm. Additionally, an SO bubble was detected in the center of cornea ( Fig. Right eye was aphakic, and the anterior chamber was completely filled with SO. Slit-lamp examination revealed circumciliary congestion, diffuse stromal corneal edema, and bullous keratopathy in the right eye. Translucent cornea, fibrous pupillary membrane, and posterior synechiae were detected. The sclera was thickened, and the intraocular contents were atrophic and disorganized. Slit-lamp examination showed shrinkage in left eye. Intraocular pressures were 14 and 5 mmHg applanation in the right and left eyes, respectively. His best-corrected visual acuity was hand movement OD and no light perception OS. Pars plana vitrectomy and 1000-centistoke SO tamponade had been performed. The last surgery (11 months prior to his presentation to the hospital), performed because of recurrent retinal detachment, was performed in a different hospital. His right eye past ocular history included 3 retinal detachment repair procedures between 20. Subsequently, he developed phthisis bulbi in the left eye. Relevant past ocular history included 4 retinal detachment repair procedures on the left eye between 19. A 56-year-old man was admitted to the hospital for decreased visual acuity in the right eye.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
